Fungal vs. Bacterial vs. Hormonal Acne: What’s The Difference?
By: Massiel Nunez 2 min readGrowing up, you may have heard the general term “acne” used to describe every type of breakout. Maybe you’ve tried different skincare products to clear blemishes but have had little success. The problem could be that you’re still thinking of all types of acne the same way when, in reality, there are many types of breakouts. A key to clearing blemish-prone skin is understanding which exact type of acne you are experiencing. Let’s discuss fungal, bacterial, and hormonal acne and dive into the main differences and how to tackle them.
Malassezia Folliculitis (AKA) Fungal Acne
You may be wondering, “What is Fungal Acne?” It’s actually not acne at all. This skin concern, also called Malassezia Folliculitis, is caused by the overgrowth of yeast (Malassezia) in the hair follicles. This results in small, often red pimple-like bumps. These bumps are typically more uniform and often appear on the forehead, chest, and back. Another distinction is that Malassezia Folliculitis tends to be very itchy. Folliculitis can also be bacterial when caused by Staphylococcus aureus bacteria. While fungal and bacterial folliculitis resemble acne, they have different underlying causes and conditions.
Types of Folliculitis
Several types of folliculitis exist, but each is unique based on its cause and specific characteristics.
According to the Mayo Clinic, the types of folliculitis include:
- Malassezia Folliculitis: Yeast (Malassezia) overgrowth results in itchy and uniform pus-filled bumps.
- Bacterial Folliculitis: This type of folliculitis appears as a rash of itchy, pus-filled bumps. It is caused when hair follicles become infected with bacteria, usually Staphylococcus aureus (staph).
- Hot Tub Rash (Pseudomonas Folicululitis): This condition results in round, itchy bumps appearing after exposure to pseudomonas bacteria in contaminated water found in pools and hot tubs.
- Razor Bumps (Pseudofolliculitis Barbae): This type of folliculitis is commonly found in people with curly hair on the face and neck. It is caused by ingrown hairs caused by close shaving.
- Gram-Negative Folliculitis: Produces pus-filled bumps around the nose and mouth, often occurring in individuals on prolonged antibiotic therapy for acne.
- Eosinophilic Folliculitis: This leads to intense itching and recurring bumps near hair follicles on the face and upper body, commonly seen in HIV/AIDS patients. The cause of this condition is still not known.
- Boils (Furuncles) and Carbuncles: Deeply infected hair follicles caused by staph bacteria that result in sudden, painful bumps or clusters of boils.
- Sycosis Barbae: Inflamed hair follicles due to shaving, particularly affecting the face.
What Causes Fungal Acne
Fungal acne is primarily caused by an overgrowth of a yeast called Malassezia on the skin. Although Malassezia is a natural resident of our skin, it can multiply and lead to fungal acne under certain conditions.
Here are some factors that can cause fungal acne:
- Oily Skin Type: Excess sebum production promotes an environment for Malassezia to thrive.
- Living in a Warm & Humid Climate: The combination of heat and humidity can create ideal conditions for yeast overgrowth.
- Taking Antibiotics: Antibiotics can often disrupt the balance of microorganisms on the skin, allowing Malassezia to grow rapidly.
- Wearing Tight-Fitting Clothing: Nonbreathable clothing can trap heat and moisture, promoting yeast growth. Opt for loose clothes. If you are wearing sweaty clothing, do not wear it for a prolonged time.
- Waxing/Shaving: Hair removal methods that irritate the skin can damage your skin barrier, making it more susceptible to fungal infections.
- Damaged Skin Barrier: Conditions such as dermatitis or eczema can weaken the skin's protective barrier, making it easier for Malassezia to cause infection.
- Exercising Without Showering Soon After: A moist environment can form as a result of sweat, which can lead to fungal growth if left on the skin.
- High Glycemic Index Diet: Sugary diets and refined carbohydrates can contribute to yeast overgrowth.
- Going in a Hot Tub or Pool: Exposure to water contaminated with pseudomonas or other bacteria can lead to folliculitis.
What Does Fungal Acne Look Like
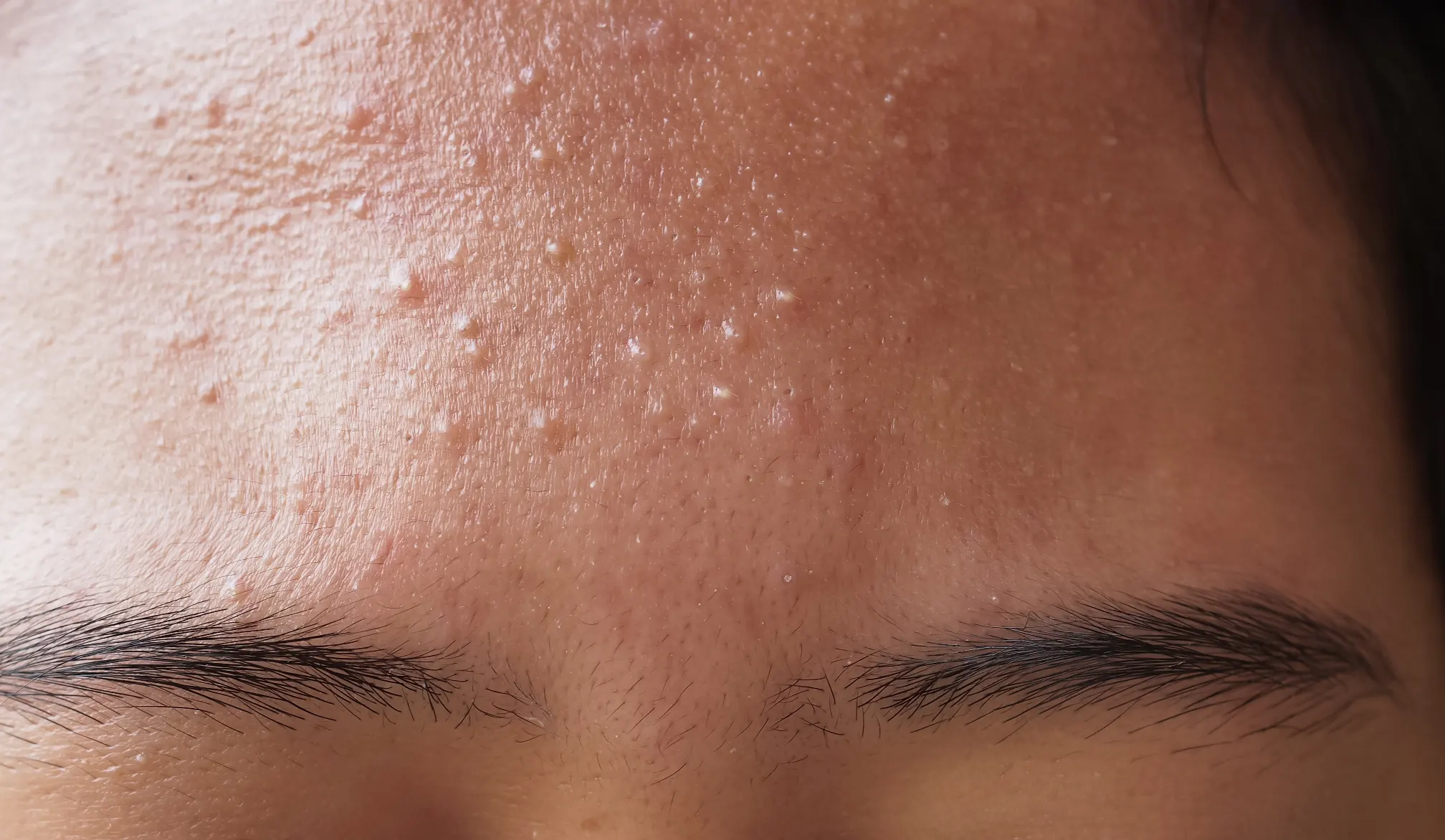
Fungal acne resembles tiny, uniform bumps clustered closely together on the skin. They often appear as a rash-like breakout. It is commonly found on the chest, back, shoulders, and sometimes on the face. The bumps are usually small (around 1-2 mm in diameter) and will appear uniform. Unlike traditional acne, fungal acne tends to be very itchy.
The bumps associated with fungal acne typically lack the larger, deeper, and more inflamed characteristics of cystic acne. Fungal acne appears as small red or skin-colored bumps that can be slightly raised. Sometimes, they resemble goosebumps. Due to the accumulation of pus, these bumps can have a slight yellowish or whitehead-like appearance.
Here is an example of what fungal acne can look like:
How is Fungal Acne Treated?
There are various ways to treat fungal acne. The goal is to eliminate the yeast overgrowth on the skin while preventing future flare-ups.
Here are some Fungal Acne treatment options:
1. Gentle Cleansing:
- Use a Gentle Cleanser: When washing your skin, opt for a mild, gentle cleanser that won't strip the skin's natural oils. Avoid harsh scrubs or exfoliants that can worsen irritation. Almond Clear’s Face & Body Wash gently washes the skin and is safe for daily use and sensitive skin.
- Keep Skin Clean and Dry: Shower after sweating and use clean towels and clothing to prevent further irritation.
2. Antifungal Products:
- Mandelic Acid Products: Mandelic Acid is a powerful but gentle antifungal ingredient that treats fungal acne by exfoliating the skin. The Level 1 Serum from Almond Clear is an excellent choice for this.
- Over-the-counter Antifungal Creams: Products containing active ingredients such as ketoconazole, clotrimazole, or selenium sulfide can effectively treat fungal acne. For optimal results, follow the product instructions.
- Antifungal Shampoos: If the fungal acne is on the scalp, an antifungal shampoo or dandruff shampoo containing ketoconazole, such as Nizoral, can help. Leave the shampoo on for a few minutes before rinsing thoroughly.
3. Avoid Certain Ingredients:
If you want to make sure that the products you are using are safe for acne-prone skin, then you can use Folliculitis Scout. The website has a tool that can help analyze product ingredients in skincare and makeup and determines if they will trigger fungal acne and other skin conditions.
- Avoid Oil-based or Comedogenic Products: Use non-comedogenic skincare and makeup products that won't clog pores and worsen fungal acne.
- Avoid These Ingredients:
- Oils: Coconut oil, olive oil, and other heavy oils.
- Fatty acids: Lauric acid, myristic acid.
- Esthers: Isopropyl myristate, isopropyl palmitate.
- Butters: Cocoa Butter, shea butter.
- Algae: Carrageenan, red algae extract.
- Some Preservatives: Potassium, cetyl alcohol.
4. Medical Interventions:
- Consult a Dermatologist: If home remedies and over-the-counter treatments aren't working, or if symptoms worsen, consult a dermatologist for personalized treatment plan recommendations.
- Prescription Antifungal Medications: When over-the-counter treatments are not working, a dermatologist may prescribe oral antifungal medications such as fluconazole or itraconazole.
- Topical Steroids: A dermatologist may prescribe topical medications such as a topical steroid to reduce symptoms in cases of significant inflammation and itching.
5. Lifestyle Changes:
- Control Sweat and Humidity: Avoid wearing tight clothing that traps sweat and moisture. Do not wear sweaty clothes for long periods of time. The humid environment can cause fungal acne to worsen. Opt for breathable clothing.
- Change Bedding Regularly: Clean pillowcases and sheets frequently.
- Shower More Frequently: Showering regularly removes sweat, dirt and oils from the skin that can cause fungal growth.
- Avoid Hot Tubs and Steam Rooms: Due to humidity and warmth, these environments can cause fungi and bacteria to grow.
What is Bacterial Acne?
Bacterial acne, also known as acne vulgaris, is the most common type of acne and is characterized by bacteria called Propionibacterium acnes (P. acnes) being present on the skin. This acne typically develops when clogged hair follicles are filled with excess oil and dead skin cells. P. acnes, a type of bacteria naturally found on the skin, thrives in these clogged pores, feeding on sebum (excess oil). The bacteria multiply and cause inflammation. As a result, this leads to the development of pimples and pustules. Bacterial acne can affect various body parts, but it is most commonly found on the face, neck, chest, shoulders, and back. These areas are where sebaceous glands are more active.
What Causes Bacterial Acne?
Understanding the underlying causes of bacterial acne is essential for figuring out how to prevent and treat it.
Here are several factors that can cause bacterial acne to appear:
1. Excess Sebum Production:
- One of the main factors causing bacterial acne is the overproduction of sebum by the sebaceous glands. Sebum is crucial in moisturizing the skin, but over-production can trigger clogged pores.
2. Follicular Obstruction:
- When excess sebum mixes with dead skin cells and other debris, it can block hair follicles. This creates an environment that encourages the growth of bacteria, particularly P. acnes.
3. Bacterial Growth:
- P. acnes is a type of bacteria that thrives in the anaerobic (oxygen-deprived) environment created by clogged pores. As these bacteria multiply, they trigger an inflammatory response from the body's immune system, leading to the redness and swelling associated with acne lesions.
4. Inflammation:
- The presence of P. acnes can clog pores and initiate an inflammatory response, which contributes to the formation of bumps.
5. Hormonal Influences:
- Hormonal changes, such as during puberty, pregnancy, menstrual cycles, or due to certain medical conditions can stimulate sebum production and contribute to acne development.
6. Genetics:
- Family history and genetic predisposition can also play a role in acne development. Individuals with a family history of acne are more likely to experience acne themselves.
7. Environmental Factors:
- Environmental factors such as exposure to certain pollutants or humid conditions can make acne worse by causing pore blockage.
What Does Bacterial Acne Look Like?
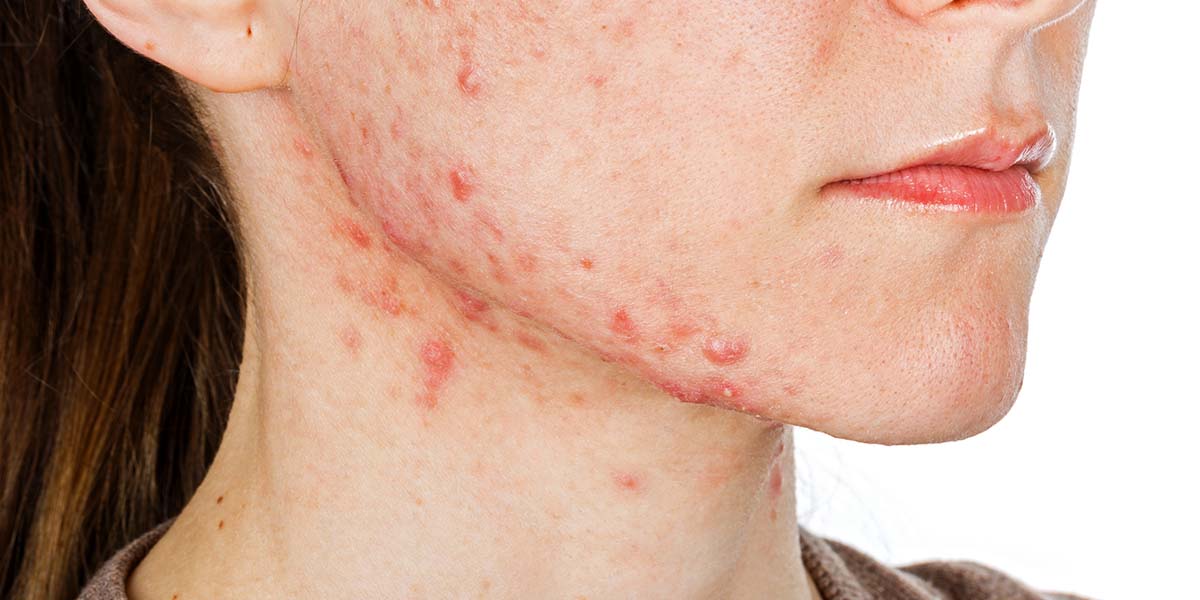
Bacterial acne can present as various types of pimples and lesions on the skin. These include whiteheads (closed comedones) and blackheads (open comedones), which result from pore blockages with trapped debris. Papules are small, red, raised bumps caused by inflammation. Pustules are similar to papules but contain visible pus. Nodules and cysts represent more severe forms of acne, with nodules being large, solid, and painful bumps, while cysts are pus-filled, deeper lesions that can lead to scarring if not treated promptly. Identifying the specific type of acne lesion is essential for determining appropriate treatment strategies.
Here is an example of what bacterial acne can look like (acne can take many formats such as cystic acne to non-inflammed blackheads and whiteheads) :

How’s Bacterial Acne Treated?
Bacterial acne is commonly treated using topical treatments and oral medications that target excess oil production, bacterial growth, and inflammation. Topical retinoids like tretinoin and adapalene help unclog pores and promote skin cell turnover. Benzoyl peroxide is effective at killing acne-causing bacteria and reducing inflammation. Salicylic acid exfoliates the skin and helps clear clogged pores.
Topical or oral antibiotics such as clindamycin and doxycycline are used to kill bacteria and reduce inflammation. In severe cases, isotretinoin (Accutane) may be prescribed to reduce sebum production and prevent acne formation, although it requires close monitoring due to potential side effects. Dermatologists may also recommend other treatments like chemical peels or laser therapy for resistant acne. Consulting a dermatologist is important to determine the most suitable treatment based on individual factors and acne severity.
What is Hormonal Acne?
Hormonal acne is a type of acne that is primarily influenced by hormonal fluctuations in the body. It commonly occurs during puberty, menstruation, pregnancy, and menopause, as well as due to certain medical conditions like polycystic ovary syndrome (PCOS).
What Causes Hormonal Acne?
Hormonal changes, particularly fluctuations in androgens (male hormones) like testosterone, can stimulate the sebaceous glands to produce sebum. Increased oil production can lead to clogged pores which creates an ideal environment for acne-causing bacteria to thrive. Hormonal acne can appear as deep, painful cysts along the jawline, chin, and sometimes the neck and back.
Causes You Can Control
Lifestyle factors can influence hormonal acne. High-stress levels can trigger hormonal changes that contribute to acne breakouts, so practicing stress-reducing activities like yoga or meditation can be beneficial. Make sure to prioritize getting enough sleep and regular exercise to help regulate your hormones and promote healthy skin.
Diet can also play a role. Excessive consumption of sugary foods, refined carbohydrates, and dairy can potentially impact your hormone levels and overall skin health. A balanced diet of fruits, vegetables, and proteins can help change your skin.
Certain medications such as birth control pills can affect hormone balance and worsen acne. You may want to consider asking your healthcare provider for alternative options. Additionally, choose skincare products labeled as non-comedogenic and avoid harsh ingredients.
Causes You Can’t Really Control
Some hormonal changes that contribute to hormonal acne are out of our control. For example puberty, menstruation, and pregnancy can alter your hormone levels. During puberty, hormonal fluctuations trigger increased oil production, leading to acne breakouts. Menstruation also causes hormonal shifts that can result in acne flare-up.
Although these hormonal changes cannot be prevented, there are still ways to manage acne. With a consistent skincare routine and treatments, you can manage breakouts.
What does Hormonal Acne Look Like?
Hormonal acne typically appears as deep, inflamed lesions on the lower face. It is especially common along the jawline and chin. The lesions typically look like large, painful, and inflamed cysts that form deep within the skin.
Additionally, hormonal acne can appear on the skin as papules and pustules, similar to bacterial acne, but they tend to be deeper and sometimes more severe. Papules are red, raised bumps without pus and pustules are inflamed lesions with visible pus at the center.
Here is an example of what hormonal acne looks like:
How’s Hormonal Acne Treated?
Treatment for hormonal acne often involves a combination of topical and oral medications that target hormone levels. A popular option is a topical retinoid. This helps unclog pores and regulate skin cell turnover. Topical or oral antibiotics also treat hormonal acne by combating bacterial growth and inflammation. Hormonal contraceptives, such as birth control pills can also be effective for managing hormonal acne by balancing hormone levels.
Be Consistent
Consistency is KEY! Many people make the mistake of only applying treatment products during breakouts. However, regular and consistent application (even when the skin appears clear) is important for long-term management. You can maintain balanced hormone activity and prevent future breakouts by being consistent.
Fungal vs. Bacterial vs. Hormonal Acne At A Glance Key Takeaways
Key Takeaways
- Bacterial Acne:
- Caused by Propionibacterium acnes.
- Characterized by whiteheads, blackheads, papules, pustules, and nodules/cysts.
- Treatment includes mandelic acid, topical retinoids, benzoyl peroxide, and oral antibiotics.
- Fungal Acne:
- Caused by excess yeast growth (Malassezia).
- Typically characterized as uniform clusters, itchy papules and pustules.
- Treated with antifungal medications and mandelic acid.
- Hormonal Acne:
- Influenced by hormonal fluctuations, especially during puberty, menstruation, and pregnancy.
- Characterized as deep, inflamed lesions on the lower face (jawline, chin), including cysts and papules.
- Treatments can involve topical retinoids, hormonal contraceptives, oral antibiotics.
Consistency in Skincare:
- Regular application of treatments, even when the skin appears clear, is essential for long-term management.
- Anti-fungal ingredients such as mandelic acid can help clear active bumps, maintain clearer skin and prevent future breakouts.