What is fungal acne?
Fungal acne- a lot of people have never heard of it, yet it’s super common (especially in warmer climates) and often mistaken for acne. Also referred to as Pityrosporum folliculitis or Malassezia folliculitis, fungal acne is actually caused by yeast that inflames the hair follicles on your skin and causes uniform, pimple-like red bumps. In contrast, the more commonly understood form of acne is inflamed by the P. acnes bacteria.
Before you get totally grossed out by the idea of yeast growing on your face or body, it’s important to know that the Malassezia yeast responsible for fungal acne is always present on the skin. We all have it! Usually your body is able to balance the yeast, fungi, and other bacteria that are also naturally part of your skin’s microbiome, but if the balance of your skin gets out of whack, an overgrowth of yeast can occur. This infects the hair follicles, which causes fungal acne. Unfortunately, once the overgrowth occurs and fungal acne gets started, it can be difficult to get it under control again. But, fear not! There are a range of treatments that can help you clear up these frustrating breakouts (more on that later).
The most common places to get fungal acne are on the chest, upper arms and back, buttocks, and especially on the T-zone area of the face, which produces a lot of oil. Basically, fungal acne can happen anywhere on the body where sweat and oil are produced. It’s important to note that If you have naturally oily skin you’re more likely to experience fungal acne. That’s because sebum (the body’s natural oil) is an excellent food source/growing medium for fungal acne. Yikes!
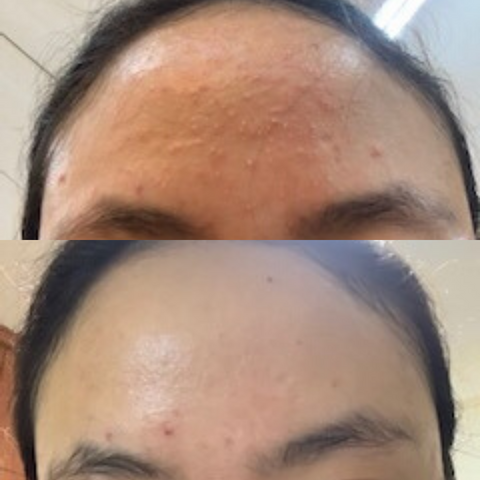
*Fungal acne before and after, forehead
What causes fungal acne?
It’s hard to say what exactly causes fungal acne because there isn’t that much research on it yet, but we’ve been able to pin down some conditions or events that might cause fungal acne to grow:
- Taking Antibiotics: Antibiotics kill bacteria in your body. Sometimes this is necessary to stop an infection, but an unfortunate side effect is that the microbiome of your skin can get discombobulated, causing Malassezia yeast to proliferate inside your pores. Unfortunately, a lot of people take oral antibiotics to treat acne, and they end up trading out one problem for another. The acne goes away (at least temporarily), but now they’ve got a bad case of fungal acne. Sometimes even doctors can’t tell the difference between fungal and bacterial acne, so they’ll continue prescribing antibiotics to treat the “acne”, thus making the fungal acne even worse and continuing the breakout cycle. This is how a lot of people end up with a mixture of both fungal acne and regular acne.
- Trapped Moisture & Tight Clothes: Most people who deal with fungal acne tend to sweat a lot, either naturally or through exercise. Wearing sweaty workout clothes, re-wearing workout clothes, or just naturally sweating in tight, non-breathable clothing can encourage yeast to grow, causing fungal acne.
- Oily skin: Both types of acne (fungal and “normal,” bacterial acne), feed off of sebum, the skin’s natural oil. If your skin is very oily, then there’s plenty of food available for the microbes that cause blemishes. This is another reason why many people suffer from both types of acne at the same time.
- Warm, Moist Environments: If you live in a place that is hot and humid where sweating is more likely, then you are much more prone to experience fungal acne because Malassezia yeast grows best in warm, moist environments. You can also get a case of fungal acne started by visiting a very warm, humid place for an extended period of time (think: extended tropical vacation). According to Google Trends, in 2021 the top three countries in the world where people search online for fungal acne information are Indonesia, Malaysia, and The Philippines, three super warm and humid countries.
- Diet: Fungi and yeast can grow on carbohydrates, so if you’re eating a diet that contains a lot of simple carbohydrates (sugar and starches), then you could cause or worsen a fungal overgrowth on your skin. This is because your sweat contains glucose and it can mirror your blood glucose levels. Higher blood sugar levels means more sugar in your sweat, which can feed fungal skin infections.
- Genetics: We’re not sure why, but some people are just genetically predisposed to overgrowths of yeast, causing fungal acne to occur more frequently.

*Fungal acne on the neck, before and after.
Fungal acne symptoms
First, it’s important to understand whether you have fungal acne or regular ol’ bacterial acne. Bacterial acne and fungal acne can look very similar and often exist together. It’s important to understand the difference because these two types of acne demand different treatments and techniques. Here are some of the main differences between regular (bacterial) acne and fungal acne:
- The overall look: Bacterial acne breakouts vary in size and predominantly appear in the form of blackheads, whiteheads, and cysts. If your breakouts are mostly blackheads and contain lots of cysts, then it’s very unlikely to be fungal acne. On the other hand, fungal acne appears as uniform, smaller red bumps and pustules. These bumps sometimes come to a head with a small amount of white or yellow pus. Every once in a while a fungal blemish will get more inflamed and turn into a full-on cyst, but most of the time the bumps stay pretty small. Also, fungal acne tends to grow in tight-knit clusters on the face, while bacterial acne is more scattered.
- Itching: Bacterial acne never itches or burns. If your bumps are itchy or sometimes feel like they’re burning, then that’s a telltale sign of fungal acne.
- Breaking out from everything: If every skincare product you use causes a breakout, then you’re most likely suffering from fungal acne. Bacterial acne responds well to the bulk of acne treatment products and is less likely to be aggravated by most of the ingredients in skincare products. Fungal acne sufferers have to be extremely careful about the personal care products that they use because many common ingredients exacerbate their breakouts. For more information on which products are ingredients are safe to use, check out this super helpful guide from Simple Skincare Science. Or you can look up the ingredients lists in your products to see if they’re safe by visiting Folliculitis Scout.
- Breakouts increasing in warm weather: Another telltale sign of fungal acne is that it fades away during the winter months only to come roaring back when the temperature and humidity increase. If your breakouts are worse in the summer then they’re likely fungal.

*Fungal acne before and after, back
How to treat fungal acne
Now for the fun part: treating fungal acne! It’s not easy figuring out which products will work and which ones will make the problem worse. Luckily we’ve assembled some treatment suggestions for dealing with fungal acne:
- Prescription antifungals: Once a doctor or dermatologist diagnoses you with fungal acne, they can write you a prescription for antifungals that are either oral (taken by mouth) or topical (applied to the skin). There are many different antifungal prescriptions to choose from, and your doctor will know which one is right for you. Antifungal medications are best taken for shorter periods of time because they can have side effects and they can throw off your body’s microbiome. After your skin clears up, you can stop taking the prescription antifungal and continue keeping the fungal acne at bay by regularly applying a mandelic acid serum or another alpha hydroxy acid (more on that below).
- Mandelic acid: Mandelic acid is an alpha hydroxy acid that’s derived from bitter almonds, and it’s one of the main, go-to skincare ingredients for clearing fungal acne. Why? Because it has strong, naturally occurring antifungal and antibacterial properties, so it does a great job of clearing up both types of acne. Mandelic acid is also naturally exfoliating, so it clears clogged follicles and pores of the sebum and dead skin cells that feed fungal acne. Also, unclogging the follicles will help prevent bacteria and fungus from finding a nice, protected home to grow inside of. Almond Clear’s mandelic acid serums are great for people who struggle with fungal acne on the face and the body. To find out more about mandelic acid, check out this article.
- Other skincare acids like azelaic acid, glycolic acid, and salicylic acid are helpful for clearing up fungal acne.
- Ketoconazole: Ketoconazole is an anti-fungal ingredient that’s primarily used to treat dandruff, but washing fungal acne-prone skin with this stuff works wonders for fighting off fungus. Using a shampoo like Nizoral on fungal acne can be very effective.
- Many people report that Sulfur applied topically to the skin can work wonders for fungal acne. That’s because it’s great at sloughing off dead skin cells and it also has strong antimicrobial properties. This brand is super affordable and has tons of loyal customers.
- Avoid the skincare products that make fungal acne worse: The Malassezia yeast that causes fungal acne is fed by most types of oil as well as a bunch of other common skincare ingredients. It’s really essential to educate yourself on which products will inflame your skin condition. Acne-safe products do not mean fungal-acne-safe! To find a huge list of fungal acne-safe skincare products, check out the super informative blog Simple Skincare Science. You can also search for fungal acne-safe ingredients at the Folliculitis Scout website.
- Clothing: After a workout, be sure to quickly change out of your sweaty clothes and hop in the shower. As we know, fungal acne thrives in humid, moist environments, so getting clean and dry is very important. If you don’t have access to a shower right away, getting out of the sweaty clothes and washing the areas of your skin that are fungal acne-prone thoroughly should work. Try wearing looser, more breathable clothing like cotton, instead of synthetic fibers like nylon and polyester. Wearing cotton and other kinds of breathable materials will help your skin dry out more quickly. If you suffer from fungal acne on the face, try wearing a headband to keep sweat off your face. If you’re dealing with fungal acne on your booty, then wearing cotton underwear instead of synthetic fibers is super important.
- Take an over-the-counter antifungal supplement: Many people report that antifungal supplements help them to keep their fungal acne under control, but it’s important to change your antifungal about every month so that your body doesn’t get too accustomed to the formula. Good antifungals include garlic extract, oil of oregano, Berberine, Caprylic acid, grape seed extract, and echinacea extract. You should consult with your doctor before taking any new supplement.
*Fungal acne before and after, chest
The big takeaway
Fungal acne doesn’t have to be such a tricky skin condition to identify and treat. The main thing to remember is that fungal acne, although similar in appearance to bacterial acne, requires a different skincare approach. If you follow the tips outlined in this article then you’ll be well on your way to saying goodbye to fungal breakouts.
*Note: all before and after pics show the results of mandelic acid serum application.
Like what you read? Want to chat about skincare with people who have the same skin concerns as you? Join our Facebook Group- Almond Clear Skincare Support.